Start with the Community: Phase 1 research is complete!

Publication Date: February 22, 2021
With generous support from our funders, The John A. Hartford Foundation, Cambia Health Foundation, and CareLab at the University of Washington, we’re moving along with an ambitious four-phase consumer research project that centers on equity using participatory design methods. The goal is to identify new messaging, communications, as well as meaningful community and/or clinical strategies to improve serious illness care experiences of at-risk populations. Specifically, we’re focusing on six subgroups: Black and Latinx adults, especially those with lower incomes; people with disabilities; older adults age 65+; people who have or have had serious illness; caregivers of someone with serious illness, and caregivers of someone living in a long-term care facility.
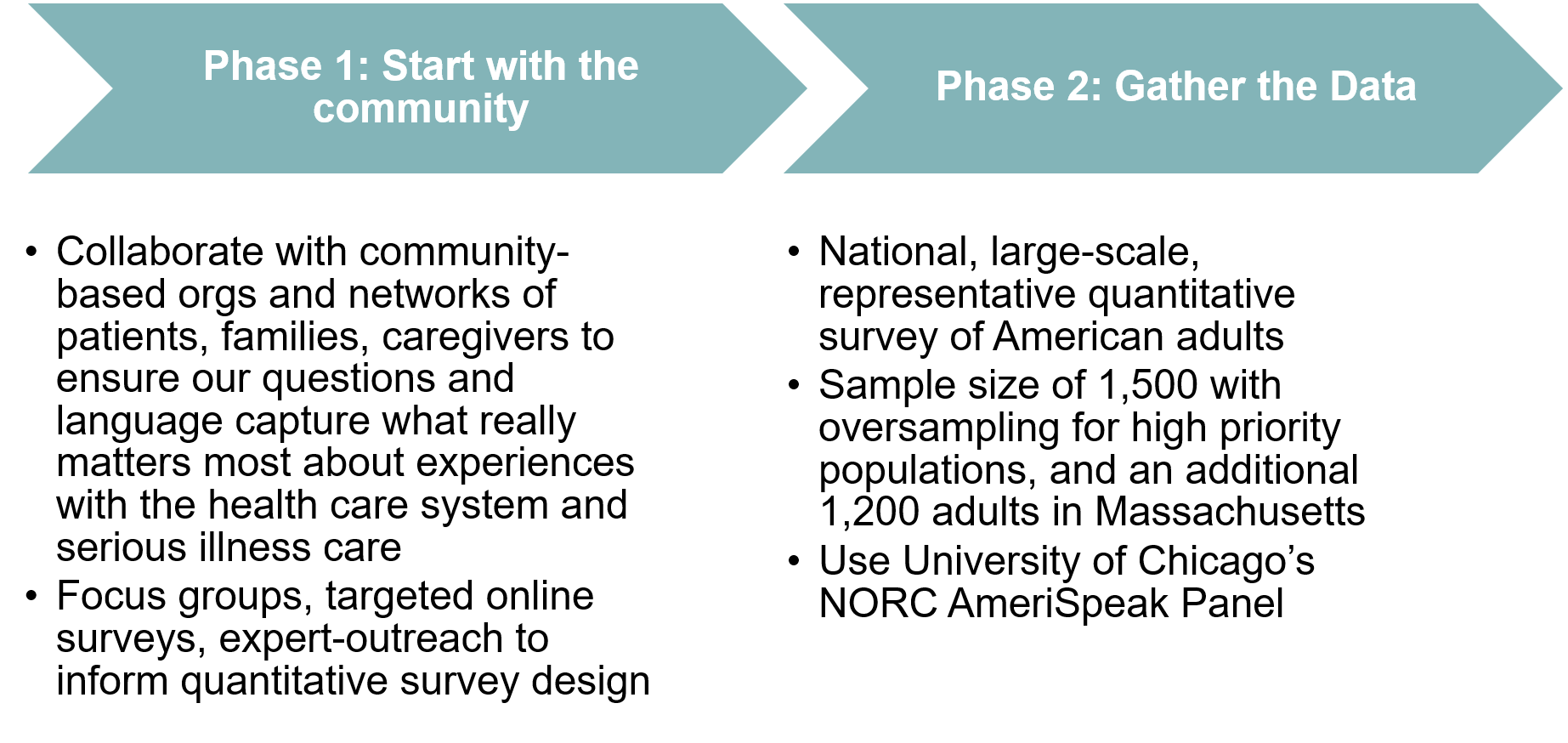
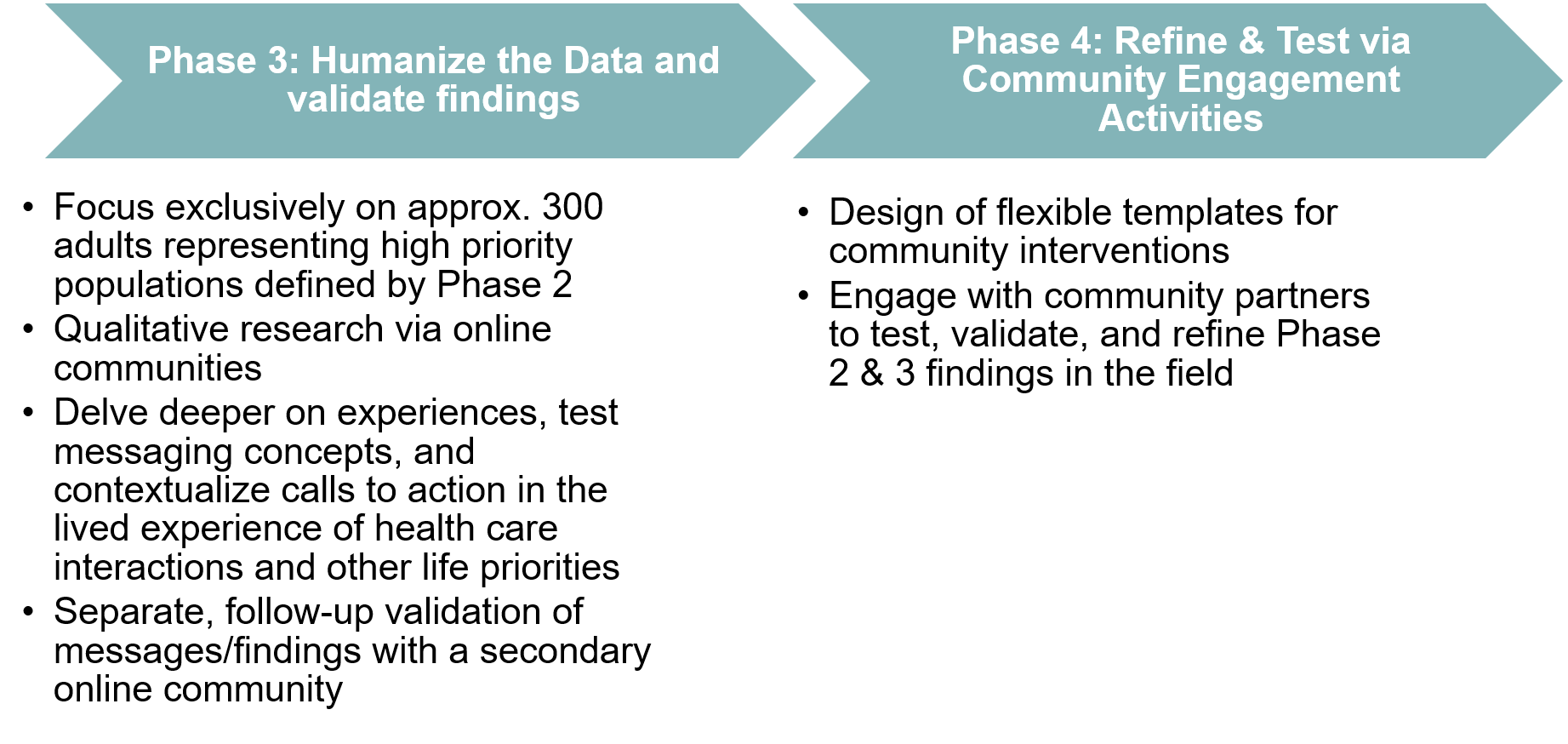
What does equity-first mean for our research?
We’re designing the research differently than we’ve ever done it before, starting with how we designed the survey questionnaire. We gathered community input on what questions to ask and the right ways to ask the questions. This included:
- Two focus groups with providers and care navigators from a community health center,
- Six in-depth telephone interviews with Black and Latinx low income older adults,
- Online stakeholder surveys with representatives from leading organizations across the country, and
- Many helpful thoughts, guidance, and feedback from Coalition members and other national leaders in translating this into actual survey questions.
What did we learn by starting with the community?
We heard rich, useful, and compelling feedback from care providers and people with lived serious illness experience. Their thoughtful responses opened our eyes to how we approached research from a position of great privilege. We wanted to share with you the most common experiences and concerns with the health care system that we heard impact how at-risk groups experience serious illness care. While none of these finding are surprising, the consistency greatly influenced the kind, amount and emphasis of our survey questions. In no particular order:
- It’s difficult to navigate the healthcare system (like referrals to multiple specialists, accessing home care, getting prescriptions refilled)
- Care is not affordable (including insurance and medications) and that impacts well-being
- They experience bias and discrimination (based on race, immigration status, age, disability, insurance coverage, etc.)
- There is not enough good quality care close by (e.g., dealing with transportation issues to get to a specialist appointment far from where they live)
- Care providers aren’t trained to help beyond immediate medical needs -- and those other needs are often much more pressing (including housing, food security, immigration status, loss of income, etc.)
Thank you!

Thank you to our generous funders: The John A. Hartford Foundation, Cambia Health Foundation, and CareLab at the University of Washington.
Thank you to Manny Lopes and the East Boston Neighborhood Health Center for its staff participation in focus groups and connecting us to older adults for in-depth interviews.
Thank you to those that provided feedback through our online stakeholder survey, and to The Conversation Project and the Coalition to Transform Advanced Care (C-TAC) for their supportive outreach in connecting us to members in their communities.
Thank you to everyone who got down into the weeds and helped translate all of our Phase 1 findings into the actual survey instrument: Rebekah Angove (Patient Advocate Foundation); Tony Back (University of Washington); Rachel Broudy (Ariadne Labs); Kate DeBartolo (The Conversation Project); Ellen DiPaola (Honoring Choices Massachusetts); Lachlan Forrow (formerly BI Lahey Health); Arlene Germain (Massachusetts Advocates for Nursing Home Reform); Marian Grant (C-TAC); Emorcia Hill (Harvard Medical School Office for Diversity Inclusion & Community Partnership); Lisa Iezzoni (The Mongan Institute); Vicki Jackson (Massachusetts General Hospital); Adriana Krasniansky (C-TAC); Rebecca Kirch (National Patient Advocate Foundation); Paul Lanzikos (Dignity Alliance Massachusetts); Alexis Levitt (Massachusetts Chapter of the National Academy of Elder Law Attorneys); James Lomastro (Dignity Alliance Massachusetts); Nathalie McIntosh (Massachusetts Health Quality Partners); Diane Meier (Center to Advance Palliative Care); Sandy Novack (Dignity Alliance Massachusetts); Cynthia Carter Perrilliat (Alameda County Care Alliance); Tyrone Pitts (C-TAC); and Shirley Roberson (C-TAC).
